Health
Peripheral Artery Disease (PAD) and Wound Healing
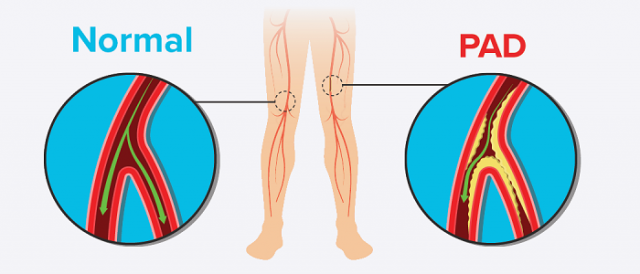
Peripheral Artery Disease (PAD) is a condition that develops when the arteries that supply blood to the internal organs, arms and legs become completely or partially blocked. This blockage is caused by fatty plaque deposits that harden arteries, called atherosclerosis, and greatly reduces blood flow.
PAD affects nearly 10 million people in the United States, especially those over 65 years of age. PAD increases the risks of hard-to-heal wounds and associated lower-limb amputations by negatively impacting circulation and reducing blood flow to and from the legs.
The Fauquier Health Wound Healing Center, located right in the town of Warrenton, identifies these risk factors for developing PAD:
- Age above 65 years
- Diabetes
- Excessive weight
- Family history of artery disease
- High blood pressure
- High cholesterol
- Heart disease
- Smoking
The Fauquier Health Wound Healing Center can also perform non-invasive tests to diagnose and accurately treat PAD. An ankle-brachial index (ABI) test is painless and easy, and compares the blood pressure reading in the ankles with the blood pressure reading in the arms. An ABI can help diagnose PAD, but it cannot identify which arteries are narrowed or blocked. A Doppler ultrasound test may be done to see which artery or arteries are blocked. Up to twenty-five percent of those with advanced PAD will experience an amputation within one year due to a non-healing wound. Although the long-term effects of PAD are serious, an astonishing 40 percent of people with PAD do not experience any symptoms.
Fauquier Health spreads awareness during the week of September 13-17, by wearing a white sock to raise awareness of PAD, chronic wounds and amputation. #WhiteSockCampaign

If you are at risk for PAD, do not dismiss leg pain as part of growing old and seek care if you have these symptoms:
- Pain or cramps in the back of your leg while walking or exercising. These pains or cramps go away when the walking or exercising stops.
- Pain in the feet or legs while resting or that wakes you from sleep.
- Decreased or no hair growth on the feet or legs.
- Lower legs and feet that are cool to touch or that have shiny skin.
- Legs and feet that appear pale when raised and bluish/purplish when hanging down.
- Weak or absent pulses in the feet
- Numbness or tingling in the feet and legs.
- A sore or wound on your toes, legs or feet that does not heal.
People who are at risk for PAD should call The Fauquier Health Wound Healing Center if they develop a wound. Specialized care provided by the center that can help to reduce healing times, increase healing rates and significantly lower amputation risks.
For more information on identifying PAD and treating chronic or infected wounds, contact Wound Care Center located at 493 Blackwell Rd., Suite 101A, Warrenton, VA 20186 or call 540.316.HEAL (4325).





























